“Unlocking the Secrets: Maternal Health and Child Neurodevelopment—Discover the Surprising Factors That Impact Your Child’s Future!”

In a recent study published in Maternal Health BMC Medicine, researchers investigated the impact of three maternal metabolic conditions—pregestational diabetes mellitus (PGDM), gestational diabetes (GDM), and obesity—on the development of neurodevelopmental conditions (NDCs) in children. The study, which explored the mediating effects of obstetric and neonatal factors on this relationship, focused on autism, intellectual disability (ID), and attention-deficit/hyperactivity disorder (ADHD).
READ: Marijuana Consumption Associated with Increased Cardiovascular Risk
Maternal Health:
The prevalence of maternal PGDM, GDM, and obesity has risen globally, paralleling an increase in NDCs, particularly ADHD and autism in children. Despite this correlation, understanding the underlying causes and developing effective preventive and treatment strategies are still in the early stages.
Maternal Health Previous research has indicated that children exposed to abnormal maternal metabolic conditions in utero face an elevated risk of NDCs due to shared genetic factors. However, there are likely additional contributing mechanisms.
Study Details:
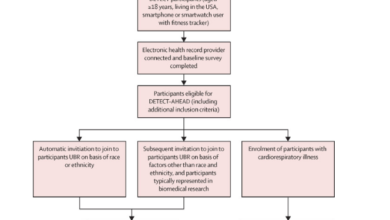
The researchers utilized data from Psychiatry Sweden, a register investigating psychiatric disorders, focusing on children born between January 1, 1987, and December 31, 2010. The study involved 2,352,969 children born to 1,299,692 mothers, with follow-up extending until December 31, 2016.
Maternal adiposity around weeks 9–10 of gestation was measured, with maternal obesity defined as a BMI ≥ 25 kg/m2. Potential mediators, such as preeclampsia, eclampsia, placental disorders, and gestational infections, were identified, and various confounders were considered in the analysis.
Analytical Approach:
The researchers employed parametric regression models for single mediation analyses and a weighting-based method for multiple mediation analyses to estimate standard errors for all mediation effect estimates. Sensitivity analyses were conducted to assess potential biases.
Results:
The study revealed that maternal PGDM had a more pronounced association with obstetric and neonatal complications, including preeclampsia, eclampsia, preterm birth, and neonatal asphyxia, compared to GDM and obesity.
The joint mediating effects of complications were more relevant during the neonatal period than during pregnancy and childbirth, particularly in the associations between PGDM and NDCs.
The mediating effects of obstetric and neonatal complications in the relationship between maternal obesity and the risk of NDCs in children were significant, though smaller in magnitude.
Conclusions:
The management of neonatal complications, especially pregnancy hypertensive diseases, preterm birth, neonatal asphyxia, and hematological comorbidities, could potentially mitigate the risk of NDCs in children, particularly in the context of PGDM.
Addressing primary metabolic factors in pregnant individuals, along with managing complications during pregnancy, childbirth, or the neonatal period, is crucial. Maternal Health Timely interventions, such as iron supplementation for infants of mothers exposed to PGDM, could offer protective measures. Overall, the study underscores the importance of a comprehensive approach to maternal health for reducing the risk of NDCs in children.